Key Takeaways for 2026 eCQM Updates
- Understand the 2026 eCQM requirements so you avoid payment adjustments and maintain full Medicare reimbursement eligibility.
- Align workflows with updated eCQM reporting standards to improve data accuracy and reduce last-minute compliance risk.
- Use certified EHR technology consistently across care teams to capture required measures and support audit readiness.
- Monitor performance throughout the reporting year so you can address gaps early and stay compliant without added operational strain.
Updated for 2026
Healthcare organizations need to stay compliant with Centers for Medicare & Medicaid Services (CMS) requirements for Electronic Clinical Quality Measures (eCQMs) and Promoting Interoperability (PI). Non-compliance can lead to financial penalties of up to 75% of the annual payment update for acute care hospitals and a 1% downward payment adjustment for critical access hospitals (CAHs).
This guide adds eCQM CMS requirements for 2026 to the updates for 2025. If you’re a healthcare administrator, compliance officer, or clinician, understanding these requirements can help keep your hospital compliant and competitive.
About IPPS, PI, and eCQM
Acute care hospitals (ACH) are paid under the Inpatient Prospective Payment System (IPPS) for Medicare inpatient stays. Instead of billing for every service, they receive a fixed payment based on the patient’s diagnosis and treatment. This system rewards hospitals for being efficient while ensuring quality care. CMS regularly updates IPPS rules, including quality reporting and Promoting Interoperability (PI) requirements.
PI programs are quality initiatives designed to improve healthcare quality, safety, and efficiency through interoperability and the use of certified electronic health record technology (CEHRT). CAHs and ACHs can participate PI defines objectives for what hospitals do with their EHRs for interoperability. PI programs include the Medicare Promoting Interoperability Program.
eCQMs are used as one component of CMS PI programs. eCQMs use data from Certified Electronic Health Record Technology (CEHRT) to assess the quality of care provided by eligible hospitals, including CAHs. Under the CMS PI Program, hospitals are required to electronically report eCQM data to CMS. While eCQM performance isn’t scored within the PI Program itself, successful reporting is required to meet program requirements. Hospitals must also achieve a minimum score across the PI objectives and measures to avoid a downward payment adjustment to their Medicare reimbursement.
What Changed for eCQM Reporting in 2026?
In addition to meeting existing CMS guidelines in 2026, ACH and CAH facilities are mandated to:
- Achieve at least 80 points on Promoting Interoperability objectives — up from 70 in 2025
- Report on eight Electronic Clinical Quality Measures (eCQMs) — up from six in 2025
Following is a breakdown of updates to help you better understand their importance and how to calculate them.
Promoting Interoperability
Interoperability in healthcare means that different systems and devices can easily share and use patient data, ensuring uninterrupted communication between hospitals, clinics, labs, and pharmacies. The outcome is that healthcare providers can quickly access accurate information to improve patient care and reduce errors.
For the 2026 calendar year, hospitals are required to report on the following interoperability objectives:
- Electronic prescribing
- Health information exchange (HIE)
- Provider to patient exchange
- Public health and clinic data exchange (with an optional bonus for using TEFCA)
- Protect patient health information (a security risk analysis and SAFER guides)
2026 also brings an added emphasis on Trusted Exchange Framework and Common Agreement (TEFCA), security, and Senior Review, All Patients, Flow, Early Discharge, and Review (SAFER) guides. Hospitals have to attest that they’ve done a security risk analysis and annual self-assessment of all eight SAFER guides.
Hospitals need to report on these objectives for any minimum 180 consecutive day period during the year. Hospitals submit data to CMS Hospital Quality Reporting (HQR). Hospitals have to use CEHRT.
Hospitals must achieve a minimum of 80 points for interoperability in 2026 and can earn up to 100 points for PI measures.
Electronic Prescribing and PDMP
Electronic prescribing is important for sharing information between healthcare systems. Hospitals need to be able to send prescriptions electronically, even for controlled substances, which require extra security steps. Part of this measure includes connecting to a prescription drug monitoring program (PDMP) through an EHR system. This integration helps ensure compliance and promotes the safe use of medications.
Scoring: In 2026, hospitals can get a maximum of 10 points for electronic prescribing and 10 points for the PDMP for a maximum total of 20 points.
Health Information Exchange Options
For 2026, hospitals can report HIE measures for:
- Using HIE bi-directional exchange
- Enabling exchange under TEFCA
- Supporting electronic referral loops by sending/receiving health information
CMS prefers that hospitals use HIEs over Consolidated Clinical Document Architecture (CCDA files). HIEs allow for real-time access to comprehensive patient information and enhance communication and coordination among healthcare providers.
Scoring: In 2026, hospitals receive a maximum of 30 points for participating in HIEs.
Provider-to-Patient Exchange
Provider-to-patient exchange means hospitals share important health information, like lab results and medication lists, directly with patients. For CMS compliance, hospitals need to ensure that patients can easily access their health records electronically through a patient portal, which encourages them to take part in their care and enhances healthcare quality.
Hospitals want to make sure patients can enroll in the patient portal during registration or discharge to empower them to take an active role in their healthcare and improve care coordination.
Scoring: In 2026, hospitals receive a maximum of 25 points for offering Provider-to-Patient Exchange.
Public Health Clinic Data Exchange
Public Health Data Exchange is about sharing health information, like vaccination records, between public health clinics and healthcare providers. To meet CMS requirements, hospitals need to set up two-way systems and must be in production with their state public health agency for the following measures:
- Syndromic surveillance reporting (required)
- Immunization registry reporting (required)
- Electronic case reporting (required)
- Electronic reportable laboratory reporting (required)
- Antimicrobial Use (AU) Surveillance measure (required)
- Antimicrobial Resistance (AR) Surveillance measure (required)
- Public health registries reporting, including cancer reporting (optional)
- Clinical data registries reporting (optional)
By sharing data, hospitals can help improve patient care and support public health initiatives in their communities.
Scoring: In 2026, hospitals receive a maximum of 25 points for Public Health Clinic Data Exchange. Hospitals can earn 5 bonus points for a “yes” response for one of the optional Public Health and Clinical Data Exchange measures.
Protect Patient Health Information
The Protect Patient Health Information objective involves doing a Security Risk Analysis (SRA) following SAFER Guides. The goal is to ensure HIPAA compliance for electronic protected health information (ePHI) by:
- Identifying vulnerabilities to ePHI security
- Ensuring that the hospital meets legal requirements for HIPAA compliance
- Take measures to find and fix security risks
- Work to prevent breaches and unauthorized access to protected patient data
SAFER guides cover 16 recommendations to secure and use an EHR.
Scoring: Hospitals are required to report a “yes” or “no” as to whether they’re meeting the measure. If a hospital doesn’t report a “yes,” it fails overall compliance.
Electronic Clinical Quality Measures (eCQMs) Updates for 2026
An Electronic Clinical Quality Measure (eCQM) is a way for healthcare providers to use electronic health record data to track and report on how well they’re delivering quality care to patients.
For the 2025 calendar year, hospitals needed to report on six specific eCQMs. Hospitals chose three of the six measures with the other three required by CMS, which focused on issues like safe opioid use and complications during childbirth.
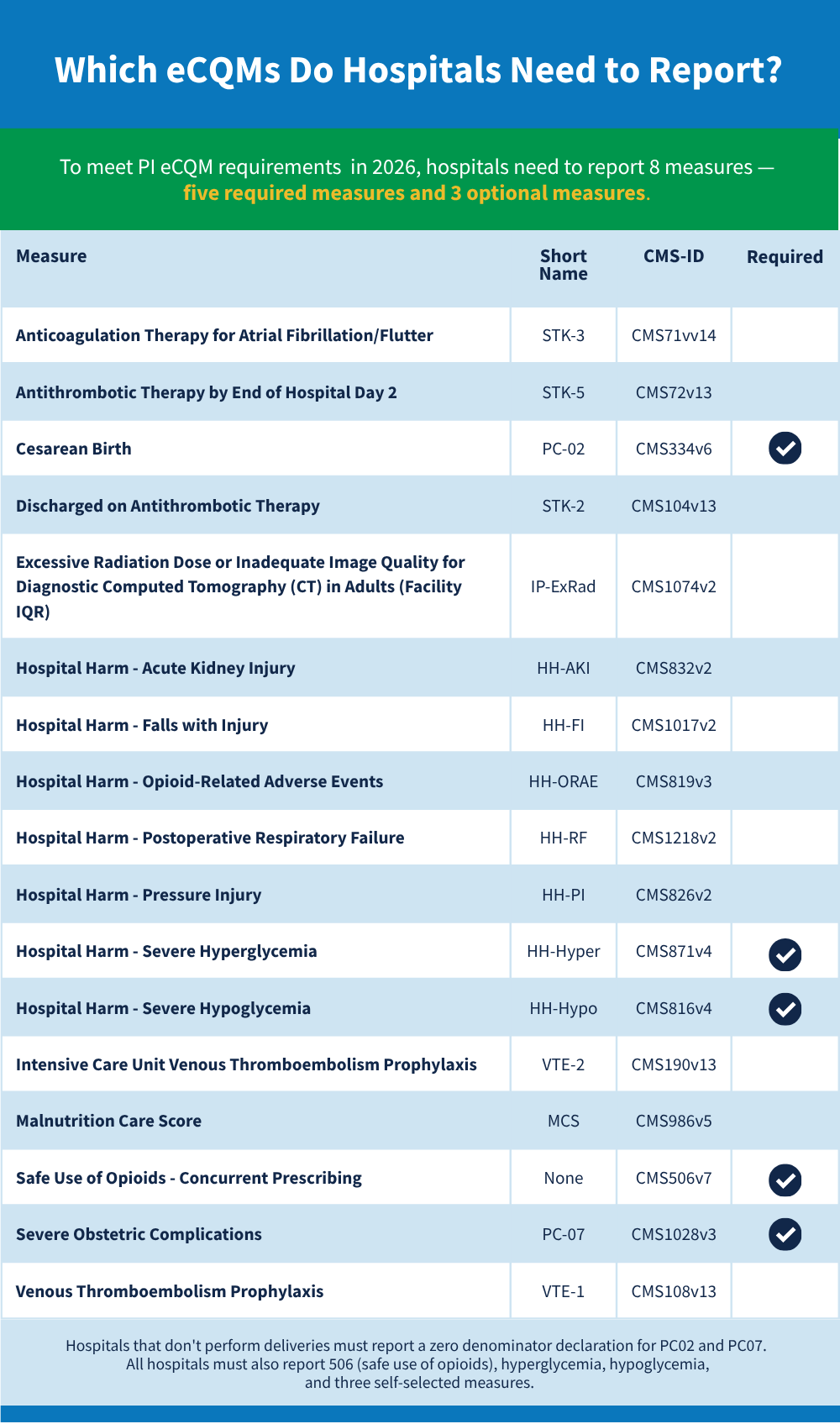
In 2026, hospitals need to report on eight eCQMs for inpatient visits. The following five are required with three others self selected from a total list of 17 (including required).
- Safe Use of Opioids – Concurrent Prescribing
- Cesarean Birth (PC‑02)
- Severe Obstetric Complications (PC‑07)
- Hospital Harm – Severe Hypoglycemia (HH‑HYPO)
- Hospital Harm – Severe Hyperglycemia (HH‑HYPER)
Note that hospitals that don’t perform deliveries must report a zero denominator declaration for PC02 and PC07. All hospitals must also report 506 (safe use of opioids), hyperglycemia, hypoglycemia, and three self-selected measures.
Preparing for Future eCQMS Requirements
CMS is expected to increase the minimum performance score for objective measures. It’s also expected to increase the number of required eCQMs to nine in 2027 and eleven in 2028.
Hospitals want to stay informed about these changes and adjust as needed.

eCQM Reporting
eCQM reports are submitted annually for the previous calendar year. Submission of eCQM files is done between January and February.
Using Technology for Compliance
Technological advancements, such as analytics and integrated EHR systems, play a big role in meeting PI and eCQM requirements. They help streamline data collection and reporting processes, reduce errors, and improve overall efficiency. By investing in the right technology, hospitals and healthcare organizations can ensure long-term compliance and enhance quality care.
EMR and EHR solutions like Azalea Health Hospital EHR help meet CMS requirements by making it easy to share patient information and track eCQMs. Hospitals can use interactive scorecards and performance estimates to track progress and identify areas for improvement. With the right tools, hospitals can ensure they meet all necessary requirements and avoid financial penalties.
In keeping with CMS requirements, the Azalea Hospital ERH:
- Is CEHRT
- Meets ONC Certification Criteria for Health IT
- Supports HL7
- Supports FHIR
Next Steps for Your Hospital to Ensure eCQM Success
Next steps for your hospital include:
- Assess your current status: Review your current compliance with CMS requirements to identify gaps, especially in achieving the minimum performance scores for interoperability and eCQMs.
- Enhance your technology: Consider upgrading or implementing an EHR system that supports interoperability and eCQM tracking. Look for solutions like Azalea Health that streamline data sharing and simplify reporting to ensure you meet CMS requirements effectively.
- Plan ahead: Create a compliance plan that outlines your strategies for meeting current and future requirements to keep your facility prepared for the upcoming changes
Sources
CDC Medicare Promoting Interoperability Program
CRISP Hospital Digital Quality Measures
eCQI Hospital – Inpatient eCQMS
eCQI Resource Center CMS Publishes 2026 Policy Changes for the Quality Payment Program
KPI-Tech Ensure 2025 Promoting Interoperability Success: Avoid Costly CMS Penalties